Hepatitis B Surface Antigen vs Antibody
Hepatitis B is a viral infection that affects the liver and can lead to both acute and chronic health issues if not diagnosed early. Blood tests play a crucial role in detecting this infection, and two of the most important markers are HBsAg (Hepatitis B Surface Antigen) and Anti-HBs (Hepatitis B Surface Antibody).
Many people find these terms confusing when reviewing their lab reports. Understanding the difference between antigen and antibody markers is essential to know whether you are infected, immune, or at risk. This blog will explain these terms in simple language to help you better understand your Hepatitis B test results.
What is HBsAg (Hepatitis B Surface Antigen)?
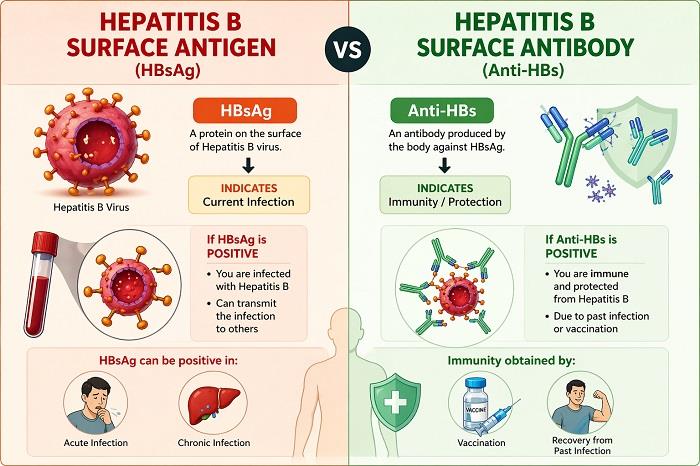
HBsAg is a protein found on the surface of the Hepatitis B virus. Its presence in the blood indicates that the virus is currently active in the body.
- Active Infection: If your HBsAg test result is positive, it usually means that you have an active Hepatitis B infection. This could be either acute (short-term) or chronic (long-term).
- Infectious Stage: A positive HBsAg result also suggests that you may be capable of transmitting the virus to others through blood or bodily fluids.
A negative HBsAg result generally indicates that there is no active infection at the time of testing. However, further tests may be required to confirm immunity or past exposure.
What is Anti-HBs (Hepatitis B Surface Antibody)?
Anti-HBs are antibodies produced by the immune system in response to the Hepatitis B virus or vaccination. These antibodies help protect the body from infection.
Immunity from Vaccination: A positive Anti-HBs result often indicates that you have developed immunity through vaccination.
Recovery from Past Infection: It may also mean that you were previously infected with Hepatitis B and have successfully recovered, gaining natural immunity.
A negative Anti-HBs result suggests that you are not immune to Hepatitis B and may be at risk of infection, especially if you have not been vaccinated.
Key Differences Between HBsAg and Anti-HBs
HBsAg indicates the presence of the virus in your body, while Anti-HBs indicates protection against the virus.
- Infection vs Immunity: HBsAg is associated with active infection, whereas Anti-HBs reflects immunity gained either through vaccination or recovery.
- Diagnostic Role: HBsAg is used to detect current infection, while Anti-HBs is used to assess immunity status.
Why Are Both Tests Important?
Testing both HBsAg and Anti-HBs together provides a complete picture of your Hepatitis B status. It helps determine whether you are infected, immune, or susceptible. Doctors rely on both markers to recommend appropriate actions, such as treatment, vaccination, or further testing.
When Should You Get Tested?
High-Risk Individuals: You should consider testing if you fall into any of these categories:
- Healthcare workers
- Individuals with multiple medical procedures
- People with a family history of Hepatitis B
- Pregnant women
Before Vaccination or Surgery: Testing is often recommended before vaccination or certain medical procedures to assess your current status.
Routine Health Checkups: Including Hepatitis B screening in routine health checkups can help detect the infection early and prevent complications.
Importance of Early Detection
- Preventing Liver Damage: Early diagnosis helps prevent complications such as liver cirrhosis or liver cancer.
- Reducing Transmission Risk: Identifying infection early allows you to take precautions and protect others.
Understanding the difference between HBsAg and Anti-HBs is essential for interpreting your Hepatitis B test results correctly. While HBsAg indicates active infection, Anti-HBs reflects immunity and protection.
Regular screening, especially for high-risk individuals, can help in early detection and timely treatment. If you are unsure about your results, always consult a healthcare professional for accurate guidance.